At Breast Imaging Matters Outreach, our mission is to empower women with clear, trustworthy breast health education.
Whether you are preparing for your first mammogram, considering breast implants, or wondering if you may qualify for earlier screening, this resource hub is designed to help you make informed, confident decisions about your breast health.
Most common general questions
-
Screening recommendations can vary based on personal risk factors and medical guidance. Many women begin routine screening around age 40, but some may qualify for earlier screening depending on family history, genetic risk, breast density, or other factors. It’s important to discuss your individual risk with your healthcare provider.
Take your personalized breast cancer risk assessment today to help you and your healthcare provider determine the screening plan that’s right for you.
-
Most women describe mammogram compression as uncomfortable but brief. Compression is necessary to gently spread out the breast tissue so clear, high-quality images can be obtained.
Each compression typically lasts only a few seconds per image, and technologists are trained to work with you to make the experience as comfortable as possible.
If you are experiencing significant pain, let your technologist know right away. Your technologist will work with you to adjust positioning and compression as appropriate while still obtaining the images needed for an accurate exam.
You are an important partner in your mammogram, and open communication helps your care team balance comfort with image quality.
-
Some women may benefit from earlier screening based on personal or family risk factors. Speaking with your healthcare provider about your individual risk is an important first step.
-
Yes. It’s important to let the imaging center know if you have breast implants when scheduling your mammogram.
Many facilities schedule extra time for patients with implants because additional images — called implant displacement views — are often needed to better visualize the breast tissue.
-
Mammograms are performed using carefully controlled compression. While implant rupture during mammography is uncommon, always inform your technologist if you have implants so proper techniques can be used.
-
Breast implants do not prevent mammograms, but they can influence how some breast tissue is visualized. Additional imaging views are typically performed to help evaluate as much tissue as possible.
-
On the day of your mammogram, avoid wearing deodorant, antiperspirant, body powder, lotion, or perfume on your chest or underarms.
Why it matters:
Many products contain tiny particles (like aluminum)
These can show up as white spots on the mammogram
They can sometimes mimic calcifications and require extra imaging
✅ Pro tip: Bring deodorant with you to apply after your exam if needed.
-
Best choice: shirt + pants, shorts, or skirt.
Most imaging centers provide a top gown only, not a full body gown.
✅ Why two-piece outfits are easier:
You only remove your top
Bottom clothing stays on
Faster and more comfortable
Less hassle in the dressing room
💡 Mammo Tech Tip: Patients in two-piece outfits almost always have a smoother check-in experience.
✔️ Also helpful to avoid
Heavy necklaces (you’ll need to remove them)
Chest powders or shimmer products
Sticky lotions on the breast area
All about Breast Density
*
All about Breast Density *
What Is Breast Density?
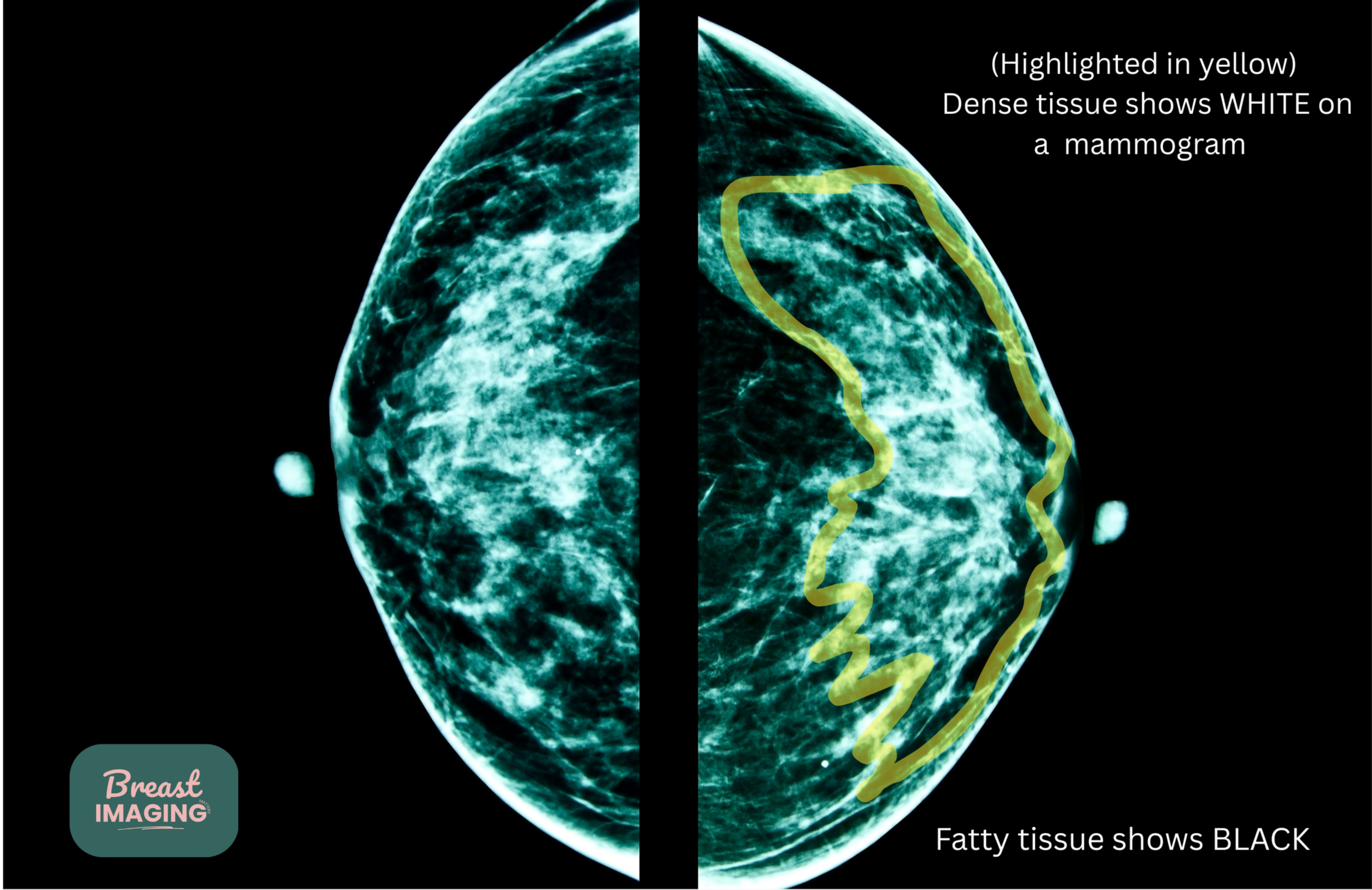
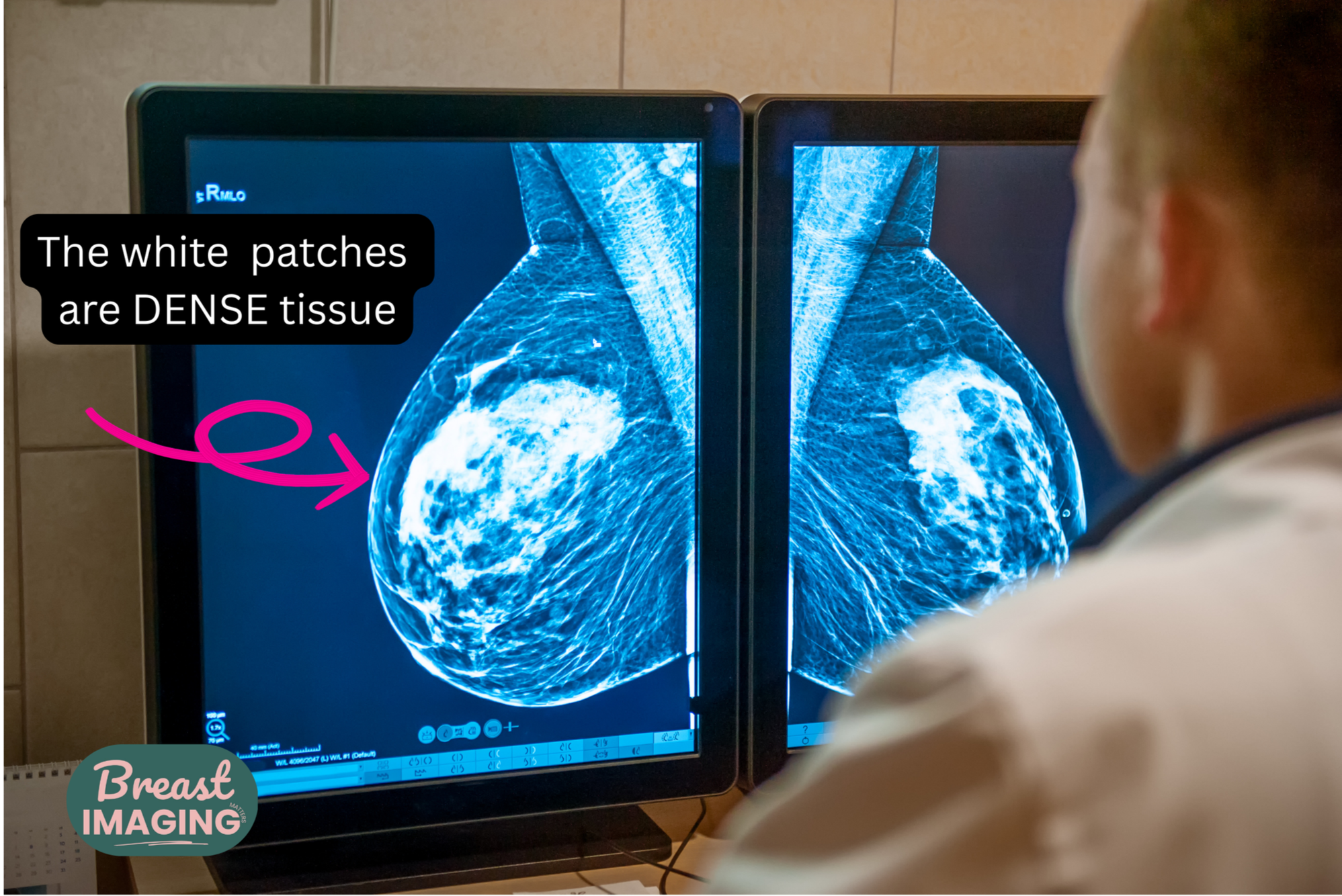
Breast density refers to the amount of fibroglandular tissue compared to fatty tissue seen on a mammogram. It is a normal and common finding.
Breast density cannot be determined by how breasts feel on exam — it is assessed by the radiologist when your mammogram is interpreted.
Breasts are typically categorized into four density groups ranging from mostly fatty to extremely dense.
How Do I Know If I Have Dense Breasts?
Your breast density is determined by the radiologist who reads your mammogram. All imaging centers include density information in the results letter sent after your exam.
If you are unsure about your breast density, you can:
✔ Review your mammogram results letter
✔ Ask your healthcare provider
✔ Contact your imaging center
Knowing your density is an important step in understanding your personal breast health profile.
Why Does Breast Density Matter?
Dense breast tissue is common, but it can make some findings more difficult to visualize on mammography because both dense tissue and many abnormalities appear white on imaging.
For some women, breast density may be one of several factors considered when discussing an individualized screening plan with their healthcare provider.
Understanding your breast density helps you ask informed questions and stay engaged in your breast health.
-
No. Dense breast tissue is very common and is considered a normal variation in breast composition.
-
Yes — breast density can change throughout a woman’s life.
For many women, breast tissue becomes less dense with age, especially after menopause. However, this is not true for everyone. Some women continue to have dense breast tissue well into their later years.
Breast density can also be influenced by factors such as:
• Hormone therapy
• Weight changes
• Genetics
• Menopausal statusBecause density can change, it’s important to review your mammogram results each year and discuss any questions with your healthcare provider.
-
Dense breast tissue is one of many factors that may be considered when evaluating overall breast cancer risk. Your healthcare provider can help you understand your individual risk profile.
-
Having dense breast tissue is common and normal. The most important next step is to stay engaged in routine screening and discuss your individual risk factors with your healthcare provider.
Breast density is just one piece of your overall breast health picture. Your provider may consider additional factors such as family history, personal history, and risk assessment when discussing your screening plan.